


Copyright © 2025 Shenyang Dasan Pharmaceutical Technology Co., Ltd.




 Posting Date:2021-12-03
Posting Date:2021-12-03 Views:
Views: Crohn's disease is an inflammatory disorder of the gastrointestinal tract characterized by an abnormal response to microbial and environmental triggers, including alterations in the microbiome dominated by Enterobacteriaceae, particularly adherent-invasive Escherichia coli (AIEC). Clinical evidence suggests that periods of psychological stress may be associated with exacerbations of Crohn's disease, and disruption of the gut microbiome is thought to be one of the underlying mechanisms. Recently, a study published in the journal Nature Communications titled “Psychological stress impairs IL22-driven protective gut mucosal immunity against colonising pathobionts” by scientists from McMaster University and other institutions has revealed a potential link between psychological stress and the onset of Crohn's disease. Using mouse models, the researchers found that stress hormones may suppress the innate immune system that normally protects the gut against invading Enterobacteriaceae—a group of bacteria, including E. coli, associated with the development of Crohn's disease.
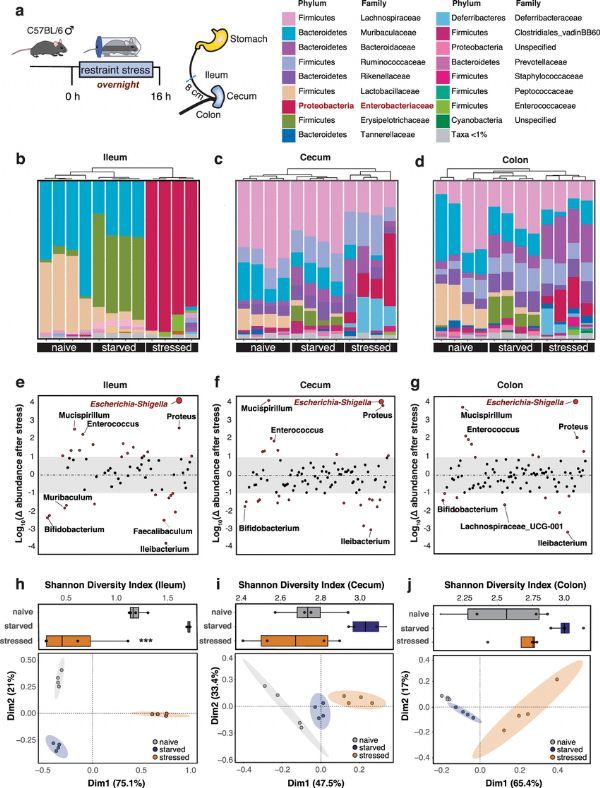
Psychological stress promotes the expansion of Enterobacteriaceae in the ileum.
Image credit: Shaler, C.R., et al. Nat Commun 12, 6664 (2021). doi:10.1038/s41467-021-26992-4
Key to innate immunity is the protective barrier of intestinal epithelial cells, which rely on molecular signals from immune cells to keep harmful microbes at bay, repair the cell wall, and secrete mucus. Without properly functioning immune cells, the epithelial barrier can break down, allowing microbes associated with Crohn's disease to invade the gut and trigger inflammatory flare-ups. Study author Professor Brian Coombes stated, "We found that psychological stress hampers the body's ability to fight off gut bacteria that are involved in the onset of Crohn's disease. Innate immunity is designed to protect us from microbes that are not supposed to be in the gut, like harmful bacteria."
When the innate immune system functions properly, it prevents harmful bacteria from colonizing the body. However, when it breaks down, it leaves an opening for pathogens to survive and cause disease in places where they normally cannot establish themselves. Professor Coombes noted that removing stress hormones in mouse models restored normal immune cell and epithelial cell function and blocked the invasion of harmful microbes. While these findings could help pave the way for new treatments for Crohn's disease, the researchers emphasize that the work remains at the preclinical stage and will require extensive further research to validate.
Crohn's disease is an inflammatory condition that causes inflammation, ulcers, and scarring in the digestive system. Although its exact cause is not fully understood, patients typically exhibit alterations in the gut microbiome, primarily characterized by changes in Enterobacteriaceae such as E. coli.
In summary, the findings suggest that immunomodulation may counteract the negative effects of psychological stress on gut immunity, offering potential avenues to improve or treat disease-associated dysbiosis.
```